Irritable Bowel Syndrome (IBS) is an often misunderstood condition that affects up to 20% of people globally. Although not life-threatening, IBS can significantly impact your daily routine, with symptoms ranging from abdominal pain to bloating, constipation, and diarrhea. However, did you know that adjusting your diet can play a crucial role in managing these symptoms? Welcome to your comprehensive guide to navigating an IBS diet.
As an Ayurvedic doctor specializing in women’s health, I understand the challenges faced by those living with IBS. It is my mission to arm you with reliable, easy-to-understand information that will empower you to take control of your IBS and live a healthier life. This guide promises to delve into the world of IBS-friendly foods, those to avoid, and special diets like the low FODMAP diet. We’ll explore specific concerns like managing IBS induced constipation and diarrhea, as well as offering tips for those aiming for weight loss. Plus, I’ll provide some delicious IBS recipe ideas to ensure you’re never short of food inspiration.
So, whether you’re newly diagnosed or a long-time IBS warrior searching for fresh insights, I invite you to join us on this journey. Together, let’s discover the best IBS diet plan tailored to your needs and start making your everyday life a little bit easier.
Understanding IBS
Irritable Bowel Syndrome (IBS) is a common gastrointestinal disorder marked by abdominal pain, bloating, and changes in bowel movements. Symptoms can range from mild to severe, and the condition can drastically differ between individuals.
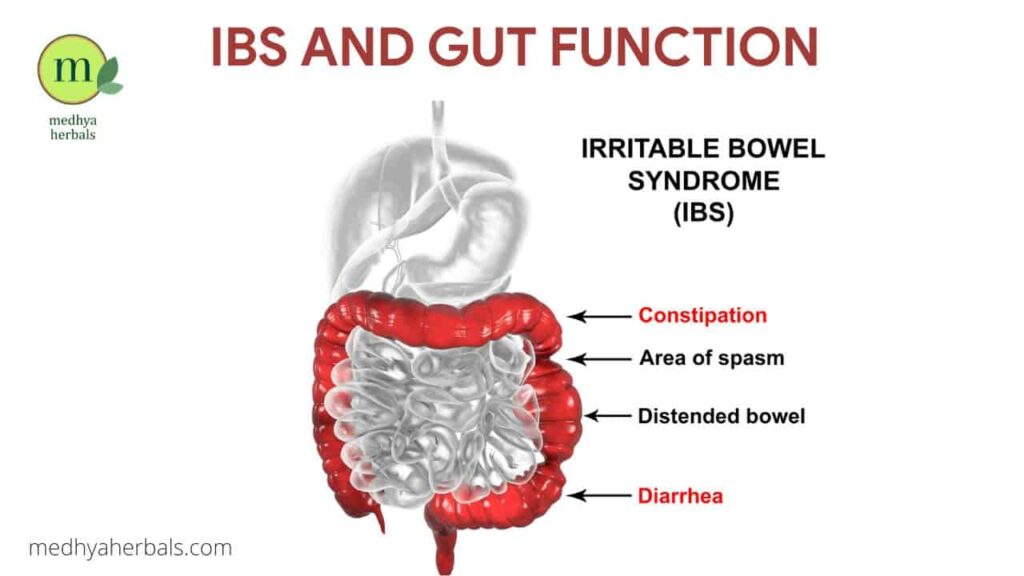
IBS has been classified into four types based on the symptoms:
- IBS-D: Dominated by diarrhea
- IBS-C: Dominated by constipation
- IBS-M: Mixed, involving both diarrhea and constipation
- IBS-U: Unsubtyped, with irregular bowel movements without a specific pattern
Causes and Triggers of IBS
The exact cause of IBS remains unknown, but several factors are believed to play a role. These include:
- Gut sensitivity: Some people have a highly sensitive gut, which can lead to overactive bowel responses.
- Gastrointestinal motor issues: Abnormalities in the speed of digestion can cause IBS symptoms.
- Low-grade inflammation: Some people with IBS show signs of inflammation in the gut.
- Changes in gut bacteria: Variations in the microorganisms in the intestines may influence IBS.
Common triggers of IBS can include certain foods, stress, hormonal changes, or certain medications.
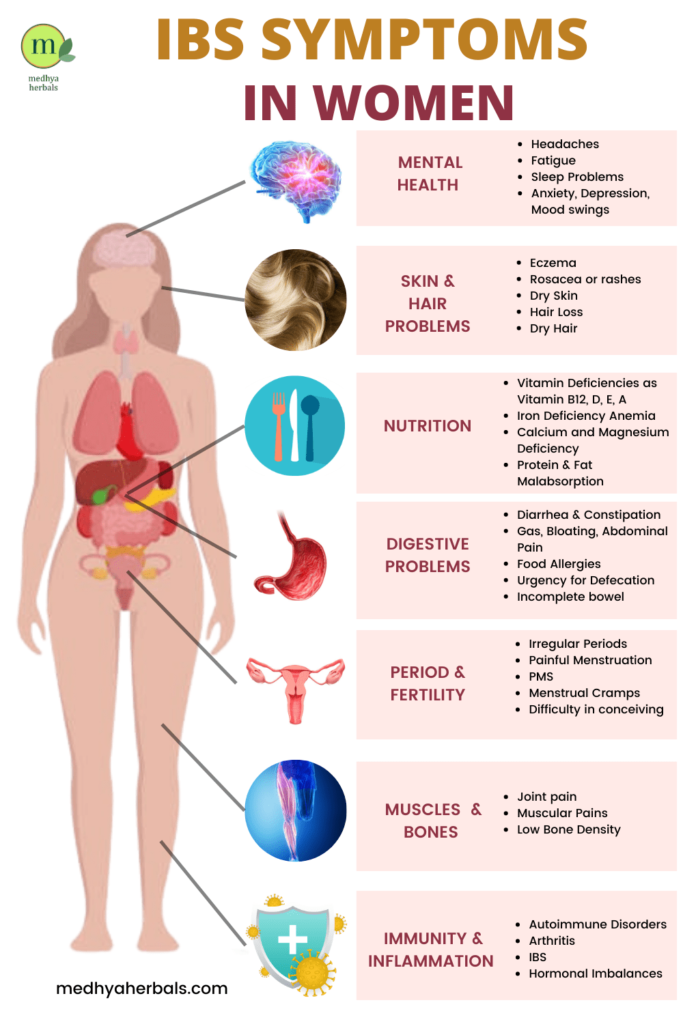
The Role of IBS Diet for Gut Health
Diet plays a crucial role in managing IBS. While it may not directly cure the disorder, a well-planned IBS diet can significantly alleviate symptoms and improve quality of life. Certain foods might trigger IBS symptoms in some individuals, whereas others might find relief from the same foods.
The relationship between diet and IBS is quite individualized, emphasizing the importance of understanding your body’s unique responses to different foods. Dietary changes, such as adopting a low FODMAP diet, reducing caffeine, or increasing fiber intake, have shown significant benefits in managing IBS symptoms.
Remember, it’s always best to consult with a dietitian or healthcare provider to guide you through the process of dietary changes for IBS. This personalized approach can help you identify your food triggers and create an IBS diet plan that suits your needs.
The IBS Diet: Foods to Include
Diet plays a pivotal role in managing the symptoms of IBS. While it’s crucial to understand which foods might exacerbate your symptoms, it’s equally essential to know the foods that can help.
Fruits and Vegetables
These are high in fiber and play a significant role in your diet. But remember, not all fruits and vegetables are created equal when it comes to IBS.
- Bananas: Yes, bananas are good for IBS. They are easy to digest and are a great source of soluble fiber, which can help manage IBS symptoms.
- Papaya: This tropical fruit is not only delicious but also beneficial for your digestive health. Papaya is known for its natural enzymes that aid digestion, making it a good choice for people with IBS.
- Carrots and Potatoes: Both are typically well-tolerated by people with IBS. They provide valuable nutrients and can be part of a balanced IBS diet.
- Cucumbers: Cucumbers are usually okay for IBS. They are low in FODMAPs and can be a refreshing addition to your diet.
However, not all fruits and veggies are IBS-friendly. For example, apples may cause issues due to their high fructose levels. As always, monitor your body’s response and adjust accordingly.
Proteins
Proteins are an essential part of your diet, and they don’t have to be off-limits because of IBS.
- Quinoa: Quinoa is a complete protein, meaning it contains all nine essential amino acids, and it’s also low in FODMAPs, making it a safe choice for individuals with IBS.
- Tofu and Tempeh: These soy products are good sources of protein, and firm tofu is considered low in FODMAPs. Tempeh, while having slightly higher FODMAP content, may still be tolerable for some.
- Chia and Hemp Seeds: These seeds are not only rich in protein but also provide a healthy dose of omega-3 fatty acids. They can be added to smoothies, cereals, and yogurt.
- Nuts (like almonds and walnuts): Nuts are a good source of protein, but they should be consumed in moderation due to their high fat content which could potentially trigger IBS symptoms.
- Salmon: This fish is not only delicious but also rich in omega-3 fatty acids, which can reduce inflammation and promote gut health.
- Prawns: Most seafood, including prawns, is usually safe for people with IBS, provided they’re not cooked with trigger ingredients like garlic or onions.
Grains
Whole grains can be a good source of fiber, but it’s important to choose the right ones.
- Rice: Yes, you can eat rice with IBS. Both white and brown rice are low in FODMAPs and typically well-tolerated.
- Sourdough Bread: This bread, particularly the spelt variety, can be easier to digest than others, making it a good choice for people with IBS.
- Oatmeal: Yes, you can eat oatmeal with IBS. Oats are a great source of soluble fiber and can be an excellent breakfast choice for those with IBS.
Remember, everyone’s reaction to different foods can vary, so it’s important to pay attention to your body and adjust your diet accordingly. The key to a successful IBS diet is personalization and balance.

Foods to Avoid in an IBS Diet
Just as certain foods can help soothe IBS symptoms, others might worsen them. These are generally known as ‘trigger foods,’ and avoiding them can be a key strategy in managing your IBS. Remember, everyone is different, so what triggers symptoms in one person may not in another. However, some foods are commonly problematic for those with IBS.
High FODMAP Foods
FODMAPs are types of carbohydrates that some people find hard to digest, leading to IBS symptoms. High FODMAP foods often trigger IBS symptoms, and avoiding them can help.
- Apples: Despite being nutritious, apples are high in FODMAPs and might trigger IBS symptoms.
- Milk: Many people with IBS are lactose intolerant, which means they might have trouble digesting the sugar in milk, leading to discomfort.
- Wheat Bread: Wheat is high in FODMAPs and can trigger IBS symptoms in some people.
Caffeinated, Carbonated, and Alcoholic Drinks
Certain drinks can stimulate the intestines and make diarrhea worse. These include:
- Coffee: Unfortunately, coffee can stimulate your intestines and increase bowel movement, making it bad for IBS, especially IBS-D.
- Carbonated drinks: These beverages can introduce gas to your digestive system and increase bloating, another common IBS symptom.
- Alcohol: It can also irritate your gut and cause diarrhea.
Processed Foods
These are often high in unhealthy fats and sugars, and low in fiber, which can aggravate IBS symptoms.
Specific Fruits and Vegetables
Some fruits and vegetables are high in FODMAPs, including:
- Tomatoes: They might cause digestive issues in people with IBS due to their high acidity and FODMAP content.
- Broccoli: This nutritious vegetable is high in FODMAPs, which can worsen IBS symptoms in some people.
- Onions and garlic: They are common triggers and are best avoided by those with IBS.
As with the beneficial foods, your response to these potential triggers can vary, so monitoring your symptoms is crucial in fine-tuning your IBS diet.
The FODMAP Diet: An Effective IBS Solution
If you’ve been looking into dietary strategies for IBS, chances are you’ve come across the term “FODMAP.” But what exactly does it mean, and how can it help manage IBS symptoms?
What is the FODMAP Diet?
FODMAP stands for Fermentable Oligosaccharides, Disaccharides, Monosaccharides, and Polyols. These are types of carbohydrates that are not fully absorbed in the gut and can be fermented upon by gut bacteria, leading to the production of gas. This process can cause bloating, gas, stomach cramps, and other IBS symptoms in some people.
The low FODMAP diet involves limiting the intake of high FODMAP foods. This diet is usually implemented in two phases:
- Elimination phase: All high FODMAP foods are avoided for a few weeks.
- Reintroduction phase: Foods are gradually reintroduced to identify which ones trigger symptoms.
Benefits of the FODMAP Diet in Managing IBS
Research suggests that a low FODMAP diet can effectively manage IBS symptoms in a majority of people. The benefits include:
- Reduction in symptoms: Many people with IBS experience fewer and less severe symptoms on a low FODMAP diet.
- Improved quality of life: With symptoms under better control, you may find you’re able to do more of the activities you enjoy.
Despite its potential benefits, the FODMAP diet is not a one-size-fits-all solution and should be customized to your individual needs. Also, the FODMAP diet can be complex because it restricts many common foods. For this reason, guidance from a dietitian can be very helpful.
It’s also important to note that the FODMAP diet is not intended to be a permanent diet. It’s more of a temporary eating pattern to identify what foods trigger your symptoms. After following the diet, most people can reintroduce most high-FODMAP foods back into their diet without experiencing symptoms.
In short, the FODMAP diet can be a powerful tool for managing IBS symptoms, but it should be undertaken with guidance and supervision.
Dealing with Constipation and Diarrhea in IBS
The primary symptoms of IBS – constipation and diarrhea – often require different dietary approaches. Although everyone’s body reacts uniquely to different foods, some general guidelines can help manage these two contrasting symptoms of IBS.
IBS Diet for Constipation
Constipation is a common symptom of IBS, characterized by infrequent bowel movements and hard, dry stools. A diet high in fiber can help manage constipation-related IBS by adding bulk to your stool and speeding up digestion.
- Increase Fiber Intake: Foods like fruits, vegetables, whole grains, and legumes are high in fiber. However, try to introduce fiber gradually into your diet to avoid bloating and gas.
- Stay Hydrated: Drinking plenty of fluids, particularly water, can help prevent dehydration, a common cause of constipation. Warm water, in particular, can aid digestion and ease constipation.
- Physical Activity: Regular exercise can also help stimulate digestion and relieve constipation.
However, remember that some high-fiber foods might be high in FODMAPs, so ensure you’re choosing the right ones for your body.
IBS Diet for Diarrhea
On the flip side, if your IBS symptoms lean towards frequent, loose stools, you might benefit from a slightly different approach.
- Low-FODMAP Diet: As mentioned earlier, a low-FODMAP diet can reduce symptoms of IBS, including diarrhea.
- Limit Fat Intake: High-fat foods can increase intestinal contractions and cause diarrhea. Reducing your intake of fatty foods like fried foods, butter, and cream might help.
- Consider Lactose: Some people find that lactose – a sugar in milk and dairy products – can trigger IBS diarrhea. You might consider limiting lactose or using lactose-free products to see if it helps.
- Soluble Fiber: While too much fiber can lead to diarrhea, the right kind of fiber can actually help. Soluble fiber, found in foods like oats and oranges, can help absorb water in the gut and form a gel-like substance, making stools firmer.
As with any dietary changes related to IBS, it’s recommended that you consult with a dietitian or healthcare provider to create a personalized plan. It’s essential to monitor your symptoms and adjust your diet accordingly. Remember, what works for one person might not work for another. Understanding your body’s unique responses to different foods is the key to managing IBS effectively.
Weight Loss and IBS: Navigating a Complex Relationship
It’s no secret that weight loss requires careful consideration of diet and exercise. However, if you’re dealing with IBS, it can feel like an added layer of complexity. But don’t worry, it’s completely possible to lose weight while effectively managing your IBS symptoms. Let’s delve into how the IBS diet can play a role in weight loss and the best practices to follow.
IBS Diet and Weight Loss
Contrary to what you might think, the IBS diet isn’t about restricting calories or certain macronutrients. It’s about choosing foods that are easy on your digestive system. That said, a diet that’s high in fiber and low in fat – a common recommendation for IBS sufferers – can also help you lose weight. Here’s why:
- Fiber: Fiber-rich foods, such as fruits, vegetables, and whole grains, tend to be low in calories. Plus, fiber can help you feel full, which can prevent overeating and aid weight loss.
- Low-fat foods: Fat is high in calories, so reducing your fat intake can help create the calorie deficit needed for weight loss.
However, it’s important to note that everyone’s body reacts differently to foods. What aids weight loss in one person might trigger IBS symptoms in another.
Best Practices for Weight Loss with IBS
If you’re trying to lose weight with IBS, here are some best practices:
- Personalize your diet: While there are general guidelines, the best diet for you is one that aligns with your body’s needs. You might find that certain low-FODMAP or high-fiber foods cause IBS symptoms, so it’s important to personalize your diet.
- Stay Hydrated: Drinking enough water can aid digestion, help you feel full, and support overall health.
- Regular Exercise: Physical activity can help you burn calories and lose weight. Plus, regular exercise can also improve digestion and reduce stress, both of which can be beneficial for IBS.
- Mindful Eating: Paying attention to what and how much you’re eating can help you lose weight. It can also help you identify any foods that might trigger IBS symptoms.
- Seek Professional Help: A dietitian can help you create a balanced, nutritious diet that considers your IBS and weight loss goals.
Remember, losing weight with IBS might require some trial and error. It’s important to be patient with yourself and to seek professional advice when needed.
Creating Delicious IBS Diet Recipes
Adopting an IBS diet doesn’t mean you have to compromise on taste. There are countless delicious and IBS-friendly recipes that you can enjoy while managing your symptoms. Let’s explore some ideas for meals that are both satisfying and gentle on your gut.
Low-FODMAP Breakfast Ideas
1. Banana and Blueberry Oatmeal: Oats are a great source of soluble fiber and are easy to digest. Top cooked oats with ripe bananas (a low-FODMAP fruit) and a handful of blueberries for a sweet and hearty breakfast.
2. IBS-friendly Scrambled Eggs: Eggs are a safe option for most people with IBS. Add some low-FODMAP vegetables, such as bell peppers or spinach, for extra flavor and nutrients.
Tasty Lunch and Dinner Recipes
1. Grilled Salmon with Dill and Lemon: Salmon is packed with protein and omega-3 fatty acids, making it a great choice for people with IBS. The herbs and lemon add flavor without adding any FODMAPs.
2. Chicken and Vegetable Stir-fry: Using low-FODMAP veggies like bell peppers, carrots, and zucchini, this dish is packed with flavor and nutrients. Just make sure to use gluten-free soy sauce if you’re sensitive to wheat.
3. Quinoa Salad: Quinoa is a great source of protein and fiber. Toss cooked quinoa with your favorite low-FODMAP veggies, olive oil, and a squeeze of lemon for a light and satisfying meal.
Delicious Snacks and Desserts
1. Homemade Popcorn: Popcorn is a low-calorie snack that’s also low in FODMAPs. It’s a great source of fiber, too.
2. Strawberries and Lactose-free Yogurt: This combo makes a refreshing and sweet snack. Just make sure to choose a yogurt that’s free of high-FODMAP sweeteners, like honey or high-fructose corn syrup.
Remember, the most important thing is to listen to your body. If a food triggers your IBS symptoms, even if it’s considered safe, you should avoid it. However, with a bit of creativity and experimentation, you can create a menu that’s delicious, varied, and IBS-friendly.
IBS Diet Plan
Here’s an example of a 7-day vegetarian IBS diet plan. This can help you to get started on following a healthy and balancing diet when Remember that each person’s tolerance may vary, so adjust as necessary. Consult a dietitian or healthcare provider for personalized advice.
Day 1:
- Breakfast: Gluten-free oatmeal with blueberries
- Lunch: Quinoa salad with bell peppers, cucumbers, and carrots
- Dinner: Baked sweet potato with spinach and feta cheese
- Snack: Banana
Day 2:
- Breakfast: Scrambled tofu with gluten-free toast
- Lunch: Lentil soup with a side of cucumber salad
- Dinner: Stir-fried tempeh with bell peppers and basmati rice
- Snack: A handful of almonds
Day 3:
- Breakfast: Chia seed pudding with a hint of maple syrup
- Lunch: Tofu stir-fry with bell peppers, carrots, and zucchini served with basmati rice
- Dinner: Quinoa-stuffed bell peppers
- Snack: An orange
Day 4:
- Breakfast: Banana and strawberry smoothie with almond milk
- Lunch: Chickpea salad (lettuce, cherry tomatoes, cucumber)
- Dinner: Baked eggplant with a side of quinoa and green beans
- Snack: A handful of walnuts
Day 5:
- Breakfast: Gluten-free pancakes with blueberries
- Lunch: Lentil salad with carrots, cucumber, and bell peppers
- Dinner: Tempeh stir-fry with bell peppers, and zucchini served with basmati rice
- Snack: A banana
Day 6:
- Breakfast: Scrambled tofu with gluten-free toast
- Lunch: Stuffed bell peppers with quinoa and vegetables
- Dinner: Baked sweet potato with a side of spinach and feta cheese
- Snack: A handful of almonds
Day 7:
- Breakfast: Chia seed pudding with strawberries
- Lunch: Tofu stir-fry with bell peppers, carrots, and zucchini served with basmati rice
- Dinner: Quinoa salad with broccoli, bell peppers, and cucumbers
- Snack: An orange
Diagnosing and Treating IBS: The Role of Diet and Beyond
While diet plays a crucial role in managing IBS, it’s only one piece of the puzzle. Let’s explore the process of diagnosing IBS, the role of diet in treatment, and when it’s time to see a doctor.

Diagnosing IBS
IBS is a complex disorder that’s usually diagnosed based on symptoms and the exclusion of other conditions. The Rome IV criteria, widely accepted by physicians, stipulate that IBS symptoms should include abdominal pain at least once per week for the last three months, along with changes in the frequency or appearance of stool.
Additional tests like colonoscopy can be used to rule out other conditions, but there is no definitive test to diagnose IBS.
The Role of Diet in IBS Treatment
Once diagnosed with IBS, one of the first lines of treatment often involves changes to your diet:
- Elimination Diet: This involves removing certain foods that are known to trigger IBS from your diet and then gradually reintroducing them to see how your body reacts.
- Low-FODMAP Diet: As we’ve discussed, this diet involves limiting foods that are high in certain carbohydrates (FODMAPs) that can trigger IBS symptoms.
- Fiber Intake: Depending on your symptoms, your doctor or dietitian may recommend increasing or decreasing your fiber intake.
While dietary changes can be highly effective in managing IBS symptoms, they’re often most successful when combined with other treatment strategies.
Beyond Diet: Other IBS Treatments
Besides diet, there are other treatments and IBS remedies that can help to manage and cure IBS symptoms:
- Herbal Supplements: Depending on your symptoms, several types of herbal supplements can be prescribed by your doctor, some examples include herbs such as fenugreek, ginger, aloevera, fennel etc.
- Probiotics: These can help restore a healthy balance of gut bacteria, which can improve IBS symptoms for some people.
- Stress Management: As stress can trigger IBS symptoms, techniques like yoga, meditation, and cognitive behavioral therapy can be effective.
When to See a Doctor
If you’re experiencing potential IBS symptoms, it’s essential to consult a healthcare provider. Not only can these symptoms be signs of other, potentially serious conditions, but they can also significantly impact your quality of life.
If you’re already diagnosed with IBS and your symptoms worsen, or if you’re losing weight without trying, experiencing severe pain, or noticing changes in your symptoms, it’s time to seek medical attention.
Remember, while diet is a crucial aspect of managing IBS, it’s not the only one. A comprehensive approach that includes diet, lifestyle changes, and possibly medication can help you live a healthier, happier life with IBS.
Conclusion
Living with Irritable Bowel Syndrome can be challenging, with symptoms often disrupting your daily life and making it difficult to enjoy the foods you love. It’s understandable to feel overwhelmed or frustrated in your quest for relief.
Ayurveda, with its holistic approach and natural remedies, can provide a powerful solution. Ayurvedic treatments aim to treat the root cause rather than just relieving symptoms, paving the way for more sustainable, long-term relief. The integration of tailored dietary changes, lifestyle modifications, and Ayurvedic herbs could potentially transform your IBS journey, helping you regain control over your health.
At Medhya Herbals, our experienced Ayurvedic doctors are committed to understanding your unique needs and providing personalized treatment plans. Why not take the first step toward a healthier, symptom-free life? Schedule a consultation with us today, and let us guide you on the path to IBS relief.
FAQ
Is coffee bad for IBS?
While some people with IBS can tolerate coffee, many find that it triggers or worsens their symptoms. Coffee is a known stimulant for the digestive system, and its consumption can accelerate bowel movements, potentially leading to diarrhea for some people. Plus, the high acidity level in coffee can irritate the gut lining, causing discomfort for individuals with IBS. If you notice that your IBS symptoms worsen after consuming coffee, it may be best to limit or avoid it.
Is potato good for IBS?
Potatoes are generally well-tolerated by individuals with IBS, making them a beneficial addition to an IBS diet. They’re a good source of carbohydrates and provide essential nutrients like potassium and vitamin C, without containing any of the FODMAPs (fermentable oligosaccharides, disaccharides, monosaccharides, and polyols) that are known to trigger IBS symptoms. However, preparation is key. Frying or serving potatoes with high-FODMAP foods or excessive fats may still lead to discomfort, so it’s advisable to have them boiled, baked, or steamed and paired with other IBS-friendly ingredients.
What triggers IBS flare ups?
IBS flare-ups can be triggered by a variety of factors which can differ from person to person. Common triggers include certain foods and drinks, particularly those high in FODMAPs like garlic, onions, beans, dairy products, and carbonated drinks. Stress and anxiety are also known to exacerbate IBS symptoms, as there’s a strong connection between the gut and the brain. Other triggers can include hormonal changes (many women report worse IBS symptoms during their menstrual periods), certain medications (like antibiotics or certain antidepressants), and lack of exercise. Identifying personal triggers is a crucial part of managing IBS effectively.
Are apples good for IBS?
While apples are rich in fiber and can be part of a healthy diet, they may not be the best choice for everyone with IBS. Apples contain high levels of fructose, which is a type of sugar that can be hard to absorb for some individuals, thus falling into the FODMAP category. Consuming high-FODMAP foods can lead to bloating, gas, and stomach pain in people with IBS. Therefore, if you find that apples trigger your IBS symptoms, it may be best to avoid them or only eat them in small portions. Always listen to your body and consider consulting a dietitian to develop a personalized eating plan.
Is sourdough better for IBS?
Sourdough bread can be a better option for people with IBS compared to regular bread. The reason lies in the fermentation process it undergoes. During fermentation, the natural bacteria and yeasts in the sourdough starter predigest the carbohydrates and gluten in the dough, which can make it easier to digest and potentially less likely to trigger IBS symptoms. That said, everyone with IBS is different, and while some may tolerate sourdough bread well, others might not. It’s important to monitor your body’s reaction and adjust your diet accordingly.
How do you stop triggered IBS?
Stopping a triggered IBS flare-up involves a multifaceted approach. First, identify and avoid your trigger foods or situations as much as possible. This could mean following a low-FODMAP diet or avoiding high-fat, spicy, or caffeinated foods, depending on your personal triggers. Second, stress management techniques like meditation, yoga, or deep-breathing exercises can help calm your body and reduce IBS symptoms. Regular physical activity is also beneficial for overall gut health. Over-the-counter medication can alleviate symptoms like bloating, diarrhea, or constipation. However, if your symptoms are severe or persistent, it’s important to consult with a healthcare professional or a dietitian who can provide personalized advice and potential medical treatments.
Is broccoli good for IBS?
Broccoli’s impact on IBS can vary greatly from person to person. On the one hand, it’s a nutritious vegetable packed with vitamins and fiber, which can aid in digestion. However, for some people with IBS, particularly those who are sensitive to certain types of carbohydrates called FODMAPs, broccoli (especially in large quantities) can trigger symptoms such as bloating, gas, and abdominal pain. It’s also worth noting that cooking broccoli may make it easier to digest, whereas raw broccoli might be more likely to trigger symptoms. As always, it’s important to pay attention to your body’s response and adjust your diet accordingly.
Is sweet potato good for IBS?
Sweet potatoes are generally a good choice for those with IBS. They are low in FODMAPs, meaning they are less likely to trigger IBS symptoms. Moreover, sweet potatoes are a great source of soluble fiber, which can aid in regulating bowel movements and reducing symptoms of both constipation and diarrhea. They also contain key nutrients like vitamin A, vitamin C, and potassium. However, as with all foods, they should be consumed in moderation and prepared in a way that doesn’t include other potential IBS triggers, like excessive fat or spices. As everyone’s IBS triggers can vary, it’s important to listen to your body’s response.
References
- “The Efficacy of Ayurvedic Medicines for Irritable Bowel Syndrome: A Systematic Review and Meta-Analysis.” Evidence-Based Complementary and Alternative Medicine, Hindawi, 7 May 2021, https://www.hindawi.com/journals/ecam/2021/6623816/.
- “Ayurvedic and Conventional Treatment for Irritable Bowel Syndrome: A Randomized Double-Blind Clinical Trial.” Journal of Ayurveda and Integrative Medicine, Elsevier, 1 Jul. 2017, https://www.sciencedirect.com/science/article/pii/S0975947617300839.
- “Efficacy of Ayurvedic treatment modalities in patients with Irritable Bowel Syndrome: A randomized controlled trial.” Journal of Ayurveda and Integrative Medicine, Elsevier, 1 Oct. 2019, https://www.sciencedirect.com/science/article/pii/S0975947619301583.
- “Herbal remedies for irritable bowel syndrome: a systematic review.” Journal of Pharmacy and Pharmacology, Wiley Online Library, 10 May 2021, https://onlinelibrary.wiley.com/doi/full/10.1111/jphp.13475.
- “The effect of yoga on irritable bowel syndrome: a systematic review and meta-analysis.” Complementary Therapies in Medicine, Elsevier, 1 Oct. 2019, https://www.sciencedirect.com/science/article/pii/S0965229919302955.
- “Effect of probiotics on Irritable Bowel Syndrome: a systematic review and meta-analysis of randomized controlled trials.” Journal of Gastrointestinal and Liver Diseases, National Institute of Health, 2019, https://www.ncbi.nlm.nih.gov/pmc/articles/PMC6738735/.
- “The therapeutic effect of Aloe vera in gastrointestinal disorders: a systematic review and meta-analysis.” Journal of Research in Medical Sciences, National Institute of Health, 2019, https://www.ncbi.nlm.nih.gov/pmc/articles/PMC6843916/.
- “Fennel and its potential beneficial effects in critical health conditions.” Journal of Food and Drug Analysis, Elsevier, 2018, https://www.sciencedirect.com/science/article/pii/S1021949817301897.
- “Peppermint oil for the treatment of irritable bowel syndrome: a systematic review and meta-analysis.” Journal of Clinical Gastroenterology, National Institute of Health, 2014, https://www.ncbi.nlm.nih.gov/pmc/articles/PMC4286770/.
- “The effect of ginger in the treatment of Irritable Bowel Syndrome: a systematic review and meta-analysis.” Journal of Functional Foods, Elsevier, 1 Jan. 2021, https://www.sciencedirect.com/science/article/pii/S1756464620307185.

