Ayurvedic treatment for Ulcerative colitis focuses on healing the ulcers of colon and restoring the health of the digestive system to relieve the symptoms and to prevent colitis flare ups going forward.
Usually the symptoms of ulcerative colitis start as gas, general discomfort, digestion problems, acidity and restlessness. This often leads to a series of self treatment, over medication with over the counter digestion aids and hence a delayed diagnosis!
And this itself creates severity of symptoms and hence difficulty in finding relief.
Ulcerative colitis can be healed and reversed when identified at an early stage. This should happen even before the visible symptoms arise. And this is what Ayurveda can help you with!
An all natural holistic system of medicine, Ayurveda guides us to identify the stage of health condition and hence specific natural treatment based on an individual’s unique symptoms.
In this post, we will go through the causes, symptoms, types of Ulcerative Colitis. We will learn how Ayurvedic natural treatment for colitis can help you to find relief from colitis symptoms and support your health in the long term. Let’s go!
What is Ulcerative Colitis?
Ulcerative colitis (UC) is a chronic inflammatory bowel disease that primarily affects the colon area of the digestive tract. High inflammation in colitis damages the protective mucus layer of the colon area leading to small ulcerations.
The inflammation usually begins in the rectum and spreads upward to the entire colon. The severity and stage of colitis depends on the extent of the damage to the mucus layer and also on the areas of colon that get affected due to inflammation.
Difference between Ulcerative Colitis and Crohn’s Disease
Usually, chronic Inflammatory Bowel Disease (IBD) is categorized into two diseases as Crohn’s Disease and Ulcerative Colitis. These two variations differ according to the symptoms. However, the line of treatment for both follows a similar approach of removing the inflammation of the digestive tract.

- Ulcerative Colitis is generally associated with episodes of flare ups with complete remission of symptoms in the interim. Crohn’s disease occurs more often with abdominal pain and chronically affects the anus area the most.
- There is gastrointestinal bleeding in Ulcerative colitis leading to bloody diarrhea. In Crohn’s disease, patients can struggle with fistulas, asymmetrical functioning and displacement of the digestive tract.
- In Crohn’s disease, there is a typical cobblestone pattern observed at multiple points of the gastrointestinal tract. It can affect any portion of GI tract from the mouth to the anus. Ulcerative Colitis is limited to the large intestine.
- In Crohn’s disease there are healthy portion of the digestive tract mixed with inflamed portion. In Ulcerative Colitis there is continuous damage of the colon area, starting from the anus.
Health Complications of Ulcerative Colitis
The severity of the complications due to ulcerative colitis may range from extensive growth of ulcers to an abnormal growth of tissues, which is a stage preceding cancer. This can give rise to cancerous growths.
Some of the high probability of health complications observed with untreated Ulcerative Colitis are listed below:
- Arthritis and more specifically peripheral arthritis that affects joints such as knees and ankles
- Spondolytis
- Eczema
- Stomatitis – Stomach infections
- Steatosis – Fatty Liver Disease
- Blurred Vision and Conjunctivitis – Eye infections
- Urinary Tract Infections
Symptoms of Ulcerative Colitis
Ulcerative colitis symptoms can be different as it is dependent on the site and severity of inflammation. Usually, most people with ulcerative colitis have mild to moderate symptoms due times of remission and acute symptoms during the flare ups.
Flare ups can occur suddenly even after long periods of remission. They can last from days to weeks. Between flare-ups, you may experience weeks, months, or years of remission.
The symptoms of ulcerative colitis may also be gone for a while as some people can have long periods of remission. And then you may experience a flare-up due to the triggers as diet and lifestyle factors.
Most common symptoms of Ulcerative Colitis are:
- Diarrhea, often with blood or pus
- Rectal pain
- Rectal bleeding — discharge of small amount of blood with stool
- Abdominal pain and cramping
- Urgency to defecate
- Inability to defecate in spite of the urgency
- Weakness and extreme fatigue
- Weight loss
- Fever
- Very slow growth in children
Types of Ulcerative Colitis
Ulcerative Colitis is usually classified according to its place of occurrence. Here are they.
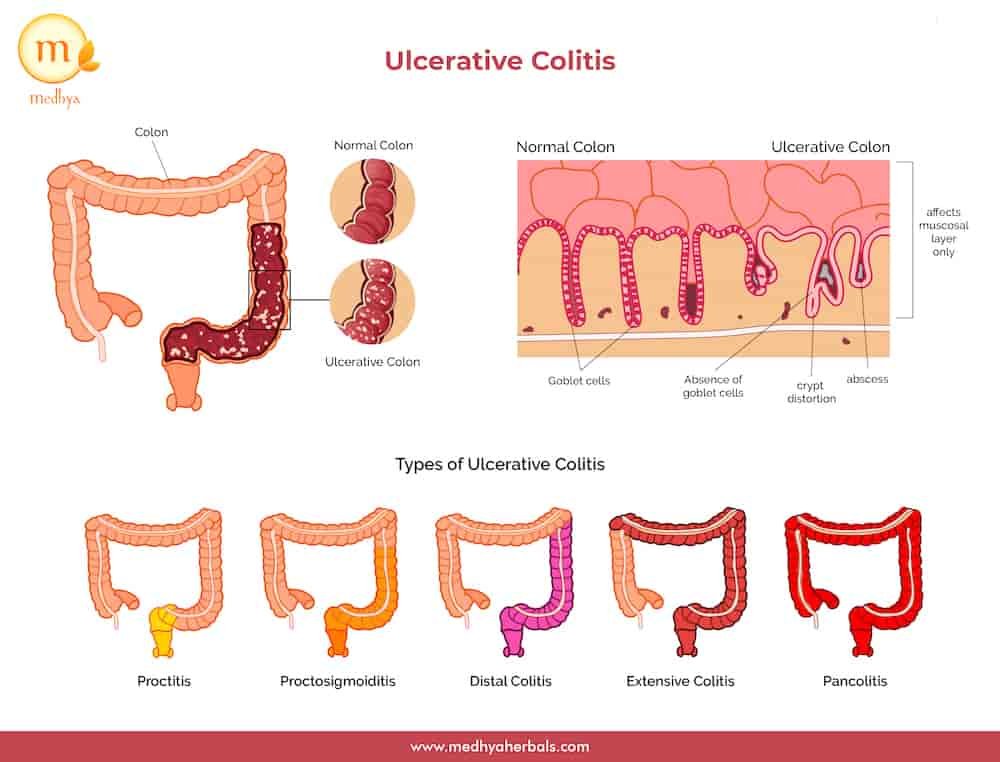
1. Ulcerative Proctitis
This type of Inflammation occurs in the area next to the anus (rectum), and rectal bleeding may be the single sign of the disease. This form of ulcerative colitis is somehow mildest.
2. Proctosigmoiditis
This inflammation involves the rectum and sigmoid colon (lower end of the colon). Symptoms are bloody diarrhea, abdominal cramps and pain, fail to pass the bowels despite the urge to do so (tenesmus).
3. Pancolitis
It is severe which always affects the whole colon and passes bouts of blood in stool in the form of diarrhea. It also causes abdominal cramps and pain, fatigue, and significant weight loss.
4. Left-sided colitis
Inflammation spreads from the rectum up through the sigmoid and descending colon. People suffer from bloody diarrhea, abdominal cramping, and pain on the left side, and quick weight loss.
5. Acute severe Colitis
This is a very rare form of colitis. It affects the entire colon and causes severe pain, more diarrhea, bleeding, fever, and inability to eat.
Causes of Ulcerative Colitis
There is no specific reason behind ulcerative colitis disease. Earlier, diet and stress were considered, but today doctors say that these may worsen the condition, rather genetics, the body’s own immune system, and the environment can cause Colitis.
1. Genetics
It has been seen that around one-fifth of people with ulcerative colitis have a family history of the same disease. Though it can be hereditary, it does not happen always.
2. Environmental, Lifestyle, and Diet
Poor diet, air pollution, cigarette smoke, and unhygienic conditions may trigger high inflammation in your body. This often creates initial stage symptoms of poor digestion and colitis beginning.
3. Auto-immune Disease
When the immune system of our body fails to fight a viral or bacterial infection, inflammation related to ulcerative colitis occurs. After this, our immune system goes on countering the ongoing inflammation.
4. Unhealthy Fats and Sugars
Linoleic acid is a fatty acid found in red meat, refined cooking oils, processed foods, fried snacks and some types of margarine. Excessive consumption of unhealthy fats and linoleic acid can creative high amounts of belly fat, which further triggers inflammation and colitis like symptoms in the body.
Similarly, excessive consumption of sugary foods and snacks triggers inflammation in the body. It undermines the health of gut flora and digestive system.
5. High Stress
Stress is one of the key triggers of poor digestion, disturbed gut flora and inflammation in the body. When you go through periods of stress, the symptoms of colitis either get flared up or can get triggered if you were prone to colitis (due to genetics or lifestyle) in the first place.
6. Medications
Certain medications, like antibiotics and non-steroidal anti-inflammatory drugs, are known to increase disease risk and trigger flares.
Ulcerative Colitis | An Ayurvedic View
Ayurveda is a natural and holistic system of medicine. According to Ayurveda, healthy digestive fire plays an integral role in our physical and mental health.
When the digestive fire is poor, Ama or toxins are produced in the body. This unwanted waste or toxin build up leads to inflammation, resulting in symptoms of Ulcerative Colitis.
Ulcerative colitis is classified as Grahani Roga of the Purushivaha Srota in Ayurveda. Grahani (the digestive tract) is the seat of agni (digestive fire), which helps in ingestion, digestion, absorption and assimilation of food. Any disturbance in the functioning of Grahani fall under the realm of Grahani Roga or the diseases of digestive tract.
Thus, when there is poor digestive fire and an aggravation of Pitta Dosha and Vata dosha in the digestive tract, it produces the classical symptoms of Ulcerative colitis.
Vitiation of Pitta, when reaches extreme will causes severe inflammation, ulceration and rectal bleeding (active phase or flare-up).
Ayurvedic Treatment of Ulcerative Colitis
Ayurvedic treatment of Ulcerative colitis is based on supporting the digestive fire, systematic detoxification and strengthening the function of the digestive tract (colon specifically).
This is achieved with Ayurvedic herbs and foods that ignite the digestive fire, enhance the assimilation of the food and remove Ama – toxins from the body.
Additionally, one may need Ayurvedic therapies such as Panchakarma that involve deep cleansing of digestive system. This helps to remove inflammation from the colon and improve its functioning.
Now, let’s look into details of Ayurvedic herbs, diet and lifestyle that can help you to achieve that:
1. Ayurvedic Herbs for Ulcerative Colitis
Ayurveda suggests suitable herbs to promote detoxification, kindle digestive fire and pacify the vitiated dosha. Provided here is a list of herbs and Ayurvedic formulations that reduce inflammation and enhance the functioning of the digestive tract.

Regular consumption of these Ayurvedic herbs helps to prevent further damage to the colon. And they also support it for regular functioning.
All the herbs and formulations that have been shared in this post are for information purpose only. All of these are potent Ayurvedic medicines that should be taken under the supervision of a qualified Ayurvedic doctor only. Do not indiscriminately use Ayurvedic herbs as it may cause more harm than benefit.
1. Triphala
This herb aids digestion. It is a combination of three herbs: Amla, Behada, and Harad. You stand to gain a lot from Triphala. Here are some health benefits:
- Boosts metabolism
- Improves bowel movement
- Detoxification of body cells
- Boosts immune system
2. Turmeric
Turmeric is a well-known blood purifier and anti-inflammatory herb It comes packed with an abundance of health benefits:
- Reduces inflammation and prevents infection.
- Strengthens the immune system against various pathogens.
- Turmeric improves the function of the digestive tract and removes toxins from the blood.
3. Giloy | Guduchi
Giloy fights inflammation. Alongside that, it has various health benefits:
- Detoxification
- Improves the function of the digestive tract
- It helps regulate blood sugar levels if consumed routinely.
- It plays a role in regulating blood pressure.
4. Kutki
A common symptom associated with ulcerative colitis is poor appetite. Kutki can remove this and improve your appetite. Here are some additional benefits of consuming Kutki:
- Enhances metabolism
- It improves digestion and absorption
5. Amalaki
Amla helps in relieving the symptoms of heat intolerance, headaches, and blood in the stools due to their Pitta Dosha alleviation properties.
6. Dadimashtaka Choorna
It improves digestion and reduces the frequency of bowels. It also helps to alleivate the vata dosha, thus relieving from symptoms of bloating and abdominal cramps.
Other herbs include Carom seeds, Neem, Shankhpushpi, Pudina, Ashwagandha, Saunf, and Brahmi.
7. Musta
Nutgrass or musta helps to improve digestion and push the toxins out of the body. It ignites the digestive fire, improves the metabolism and absorption of nutrients.
8. Nagakesara
It helps to reduce the frequency of bowel and to enhance the appetite. The Stambhana (stops bleeding) property of Nagakesara helps to end blood in the stools.
2. Ahara: The Best Diet to Heal the Colon
Your diet goes a long way to determine the health of your colon and overall digestive tract. In this case, you want to support gut health and reduce inflammation. Therefore, plan your diet with that in mind.
Best foods and food habits for Ulcerative Colitis
- Include lots of fruits, vegetables, legumes, and fibers in your diet. Eat them fresh. Take beans, peas, and other edible seeds. They are a rich source of antioxidants and can cut down the inflammation in the body.
- Focus on green leafy vegetables, variety of colors and cooling herbs and spices in your meals.
- Eat healthy meals regularly, and at the right times.
- Favor ghee, nuts like almonds, walnuts, pecans, flax seeds, sunflower seeds and pumpkin seeds, buttermilk, avocado, beets, lentils. They contain ample of prebiotics to support gut flora and healthy digestive fire.
- Focus on increasing intake of root vegetables as sweet potato and yams. They are rich in antioxidants and also balance Vata and Pitta dosha.
- Reduce your consumption of red meat, dairy, seafood and deep-fried foods.
Worst Foods to avoid for Ulcerative Colitis
- Red peppers, green onions, red wine, wheat, and cow’s milk are some examples of foods that trigger poor digestive fire and aggravate colitis symptoms.
- Avoid sugar, processed foods and artificial sweeteners in your diet.
- Fried and greasy foods lead to the production of cholecystokinin hormone that induces contractions in the colon and hence making the pain or symptoms of Colitis worse.
- Avoid irritants such as caffeinated drinks – coffee and tea, Soda, Alcohol, and Nicotine.
- Avoid chewing gums, mint, and tobacco products that introduce excess air into the body through the digestive tract.
3. Manage Stress
High levels of mental stress and health conditions such as anxiety and depression are related with poor liver health and digestive problems. In Ayurveda, we do not really separate mind and body.
In fact, Ayurveda states that our mental health is what controls our physical body. That’s why Ayurveda prescribes detailed lifestyle practices and daily routines to manage both physical and mental health.
Manage and lower stress by:
- Deep breathing exercises and yogic breathing
- Spending time in nature and with your loved ones
- Remove and reduce stress triggers
- Take time off and invest in self care measures
- Deep body massage
4. Sleep Well
Sleep deprivation affects liver health and fat metabolism. It has been studied that merely 6 hours of sleep loss in a day can significantly disturb your gut flora, blood sugar and stress levels.
Ayurveda suggests the same. Sleep is an essential pillar to health and balance in Ayurveda. And there are ample of guidelines to maintain sleep hygiene.
5. Remove Environmental Toxins
Prevent exposure to environmental toxins and body toxins by practicing a healthy lifestyle.
- Avoid all plastics and processed foods, which lead to buildup of toxins in the body.
- Get rid of chemicals based personal care and household products that deposit toxins in your system.
- Practice Ayurvedic detox or Panchakarma to clear off the toxins with Ayurvedic herbs and therapies.
- Remove stimulants such as alcohol and smoking that load your body’s detox pathways.
6. Best Lifestyle tips for a Healthy Gut
Your digestive fire health depends to a large extent on the choices you make every day. Therefore, if you want to have and maintain healthy gut, you must live like it. So, what can you do?
- Regularly practice abhyanga (self-massage). Massage improves circulation in the body. It also promotes release of neurotransmitters and hormones that relax the mind and nervous system. This allows your entire body to relax and muscles to be less tense.
- Make healthy diet choices as per above recommendations.
- Regular Exercise to tone up and strengthen the muscles of the abdominal cavity and support the digestive system functioning. It also relaxes your mind and promotes detoxification of the body.
- Control stress and anxiety.
- Get a good night’s sleep. Always make sure that you are catching on 7-8 hours of sleep in between 10 PM to 6 AM daily.
- Quit smoking and avoid alcohol.
- Cut back on added sugar and refined carbs.
- Practice meditation and deep breathing exercises (pranayama). Make sure you include meditation and pranayama in your daily routine (specifically in the morning) to relax your body and manage your gut health.
Conclusion
The symptoms of Ulcerative colitis are painful and they do make life miserable. Yet, you should know that it is possible to heal your gut and remove the source of inflammation by making simple changes in your diet and lifestyle.
The key is to start early! This is because colitis is progressive in nature. You should start small and keep building up your healthy lifestyle practices on top of one another to create a strong support for your gut health.
So start today! Do write to us for any queries and feedback. If you have tried any of the above natural approaches for ulcerative colitis, then do share your experience with us. We will get back to you the soonest.
Wishing you vibrant health!
References
Hopkins Medicine – Introduction to Ulcerative-Colitis
Orphanet – UC

