PCOS and Thyroid Disorder are two of the most common hormone imbalance disorders in women. If you’re among the millions of women who struggle with Polycystic Ovary Syndrome (PCOS) or thyroid disorders, you may be surprised to learn that there is a relationship between Polycystic Ovary Syndrome (PCOS) and thyroid function. PCOS can affect thyroid hormone levels and vice versa.
Thyroid hormones play a vital role in regulating metabolism, which affects the reproductive system, including ovulation and menstrual cycles. Women with PCOS may have a higher risk of thyroid dysfunction, such as hypothyroidism (underactive thyroid) or Hashimoto’s thyroiditis, which can worsen PCOS symptoms, including irregular periods, weight gain, and infertility.
On the other hand, changes in thyroid hormone levels can affect PCOS. Hypothyroidism can cause changes in menstrual cycles and fertility, and can also worsen insulin resistance, a common feature of PCOS.
In this post, we dig into how PCOS and thyroid disease are related to each other. What causes what? And explore the Ayurvedic treatments that can help you achieve hormonal balance and overall well-being.
What is PCOS?
Polycystic ovary syndrome, commonly referred to as PCOS, is a hormonal disorder that can cause the ovaries to become larger in size. Women with PCOS may have small cysts on the outer edges of their ovaries. While the exact causes of PCOS are not fully understood, both genetic and environmental factors may contribute to the condition.
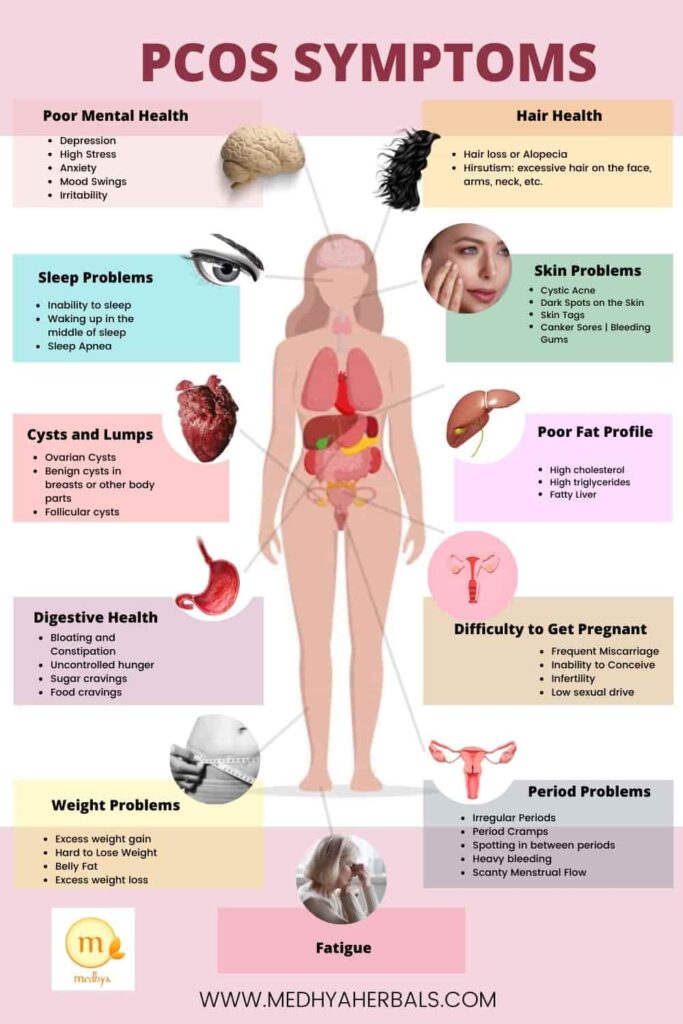
PCOS Symptoms
Symptoms of PCOS may include weight gain, irregular menstrual cycles, infertility, dark patches on the skin, and excess hair growth.
- Anovulation (inability to produce eggs);
- Infertility;
- Menstrual irregularities
- Weight gain (obesity);
- Cysts on the ovaries;
- Acne on face and back
- Excessive hair growth on the face
- Thinning of scalp Hair
- Thick or pigmentation of the skin and on the neck
- Irritability or depression
- Long terms health complications like:
- Endometrial hyperplasia.
- Endometrial carcinoma.
- Diabetes mellitus.
- Cardiovascular disease.
- Hypertension
- High blood cholesterol
Understanding Thyroid Disorders
The thyroid gland is a butterfly-shaped gland located in the neck that produces hormones that regulate metabolism. The two main hormones produced by the thyroid gland are thyroxine (T4) and triiodothyronine (T3), which help to control how the body uses energy, how fast the heart beats, and how quickly the body processes food.
The thyroid hormones produced by the thyroid gland play a crucial role in regulating metabolism, which affects many aspects of overall health. A healthy metabolism helps to maintain a healthy weight, balance blood sugar levels, and support energy levels.
Thyroid Symptoms
If there is a thyroid disorder, your metabolism could speed up excessively, or become so slow that you even begin to move slowly yourself. In the case of hypothyroidism, metabolism slows down because of an under active thyroid gland. You produce too little thyroid hormones, and this manifests as several symptoms that include:
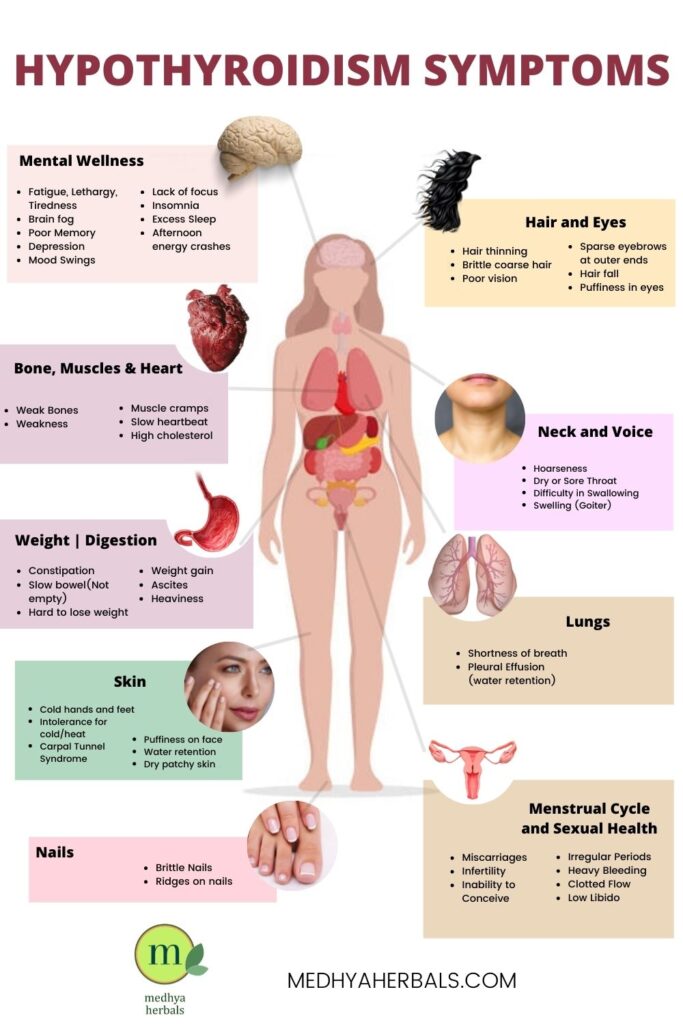
- Fatigue
- Weight gain
- Feeling cold when others are hot
- Joint and muscle pain
- Constipation
- Puffiness in the face
- Dry and thinning hair
- dry skin
- decreased sweating
- heavy or irregular menstrual periods
- impaired fertility
- depression
- reduced heart rate
Pretty much every part of your body is affected. After all, you are a sum total of your metabolic processes.
Finding the Connection between PCOS and Thyroid
While PCOS does not directly cause thyroid issues, studies have shown that women with PCOS are more likely to develop thyroid disorders, particularly hypothyroidism. This may be due to hormonal imbalances, inflammation, and insulin resistance, which are common in PCOS patients.
Hashimoto’s Thyroiditis and PCOS
Hashimoto’s thyroiditis is an autoimmune disorder that affects the thyroid gland, leading to inflammation and damage of the thyroid tissue. This can cause an underactive thyroid gland (hypothyroidism), which can result in symptoms such as fatigue, weight gain, hair loss, and depression.
A study that was completed in 2013 showed that women with PCOS are three times more likely to have this autoimmune problem that affects the thyroid gland. Four in ten women with Hashimoto’s disease also have PCOS.
While Hashimoto’s thyroiditis and PCOS are distinct conditions, there are some potential connections between them:
- Hormonal imbalances: Both Hashimoto’s Disease and PCOS can disrupt the normal hormonal balance in a woman’s body, leading to a range of symptoms. For example, hypothyroidism caused by Hashimoto’s can lead to changes in menstrual cycles as irregular periods and heavy menstrual bleeding. Similarly, excess androgens caused by PCOS can affect the menstrual cycle in women leading to anovulatory cycles, hence missed periods followed by heavy periods with clots.
- Insulin resistance: Insulin resistance, a common feature of PCOS, can exacerbate thyroid disorders by increasing inflammation in the body. This chronic inflammation can further impair thyroid function and contribute to the development of autoimmune thyroid diseases like Hashimoto’s thyroiditis. This can lead to difficulty losing weight and an increased risk of diabetes.
- Inflammation: Both Hashimoto’s and PCOS are associated with chronic inflammation in the body. Inflammation can exacerbate the symptoms of both conditions and increase the risk of complications.
Hormone Imbalances in PCOS and Thyroid
The thyroid hormones and the hormones involved in polycystic ovarian syndrome interact with each other. These interactions could be direct or indirect.
All cells in your body depend on thyroid hormones to function properly. So, certainly, thyroid malfunction affects the functioning of the reproductive system also. And this can increase your chances of having PCOS.
Excess Androgens
When you have low levels of thyroid hormones in your body, it can cause an increase in Testosterone (the most common androgen). It does this by reducing the number of sex hormone-binding globulin (SHBG).
On a normal day, this SHBG binds with Testosterone and clears it out of the bloodstream. But in this case, the number of the SHBG has gone down, leaving the Testosterone free to run around. This is similar to what happens in PCOS.
When this happens in hypothyroidism, however, it leads to PCOS symptoms. If the patient already has PCOS, then the symptoms become worse.
High LH:FSH Ratio
LH is the Luteinizing Hormone. It has the responsibility of stimulating ovulation. That is, it causes an egg to be released from a mature follicle. On the other hand, FSH, the Follicle Stimulating Hormone, is responsible for maturation of the follicles to eggs.
However, when the ratio of LH to FSH is above 3:1, there is a problem. Eggs will be released faster than they can mature. So, there are many immature follicles (things that eggs grow in) on the ovary. This ratio is a big problem in PCOS. But guess what? Hypothyroidism can also play that trick.
When the thyroid is under active, the levels of prolactin and thyroid-stimulating hormone (TSH) increase. High Prolactin levels goes on to worsen the LH:FSH ratio, thus resulting in an ovulation and menstrual cycle problems.
The Potential Link Between PCOS and Thyroid Cancer
Some studies have found that women with PCOS have a higher prevalence of thyroid nodules, which can be a risk factor for thyroid cancer. This increased risk may be due to hormonal imbalances, insulin resistance, and inflammation associated with PCOS, which can contribute to the development of various cancers, including thyroid cancer.
Hormonal Imbalances and Cancer Risk
PCOS is characterized by hormonal imbalances, such as elevated levels of estrogen and luteinizing hormone (LH). These imbalances can stimulate the growth of thyroid leading to the development of thyroid nodules and, in some cases, thyroid cancer. Additionally, insulin resistance, a common feature in women with PCOS, can lead to higher levels of insulin-like growth factor-1 (IGF-1), which has been linked to an increased risk of certain cancers, including thyroid cancer.
Inflammation and Cancer Risk
Chronic inflammation is another factor that may connect PCOS to thyroid cancer. PCOS is often accompanied by low-grade inflammation, which can cause oxidative stress and damage to cells, increasing the risk of cancer development.
Symptoms of PCOS Thyroid
Polycystic ovary syndrome (PCOS) and thyroid disorders share several common symptoms, which can make it challenging to determine the underlying cause of symptoms. Though these symptoms might even arise by different means, they could still result in the same health issues.
- Fatigue: Both PCOS and thyroid disorders can cause fatigue and low energy levels, which can impact overall quality of life.
- Weight changes: PCOS can lead to weight gain or difficulty losing weight, while thyroid disorders can cause either weight gain or weight loss.
- Irregular periods: Women with PCOS may experience irregular periods or absent periods, while thyroid disorders can cause changes in menstrual cycle length and flow.
- Thinning hair or hair loss: Both PCOS and thyroid disorders can cause hair loss or thinning hair, which can be distressing for many women.
- Mood changes: Women with PCOS and thyroid disorders may experience mood changes, including depression and anxiety.
- Infertility: Both PCOS and thyroid disorders can interfere with fertility, making it more difficult for women to conceive.
- Insulin resistance: PCOS can cause insulin resistance, which can lead to type 2 diabetes. Thyroid disorders can also impact blood sugar regulation and increase the risk of developing diabetes.
How to Heal PCOS and Thyroid Problems Naturally?
The first and most vital step is getting the proper diagnosis. As you have observed, these two conditions share a lot of symptoms. That’s why, it is possible to think that you have PCOS, when actually you have hypothyroidism.
For some women, the problems might not even show up till they try to get pregnant. In either case, early detection and prompt management are key. Here are some diet and lifestyle tips manage your health and hormone balance with PCOS and Thyroid:
1. PCOS and Thyroid Diet: Foods to Take
Improving your diet can help you in eliminating both PCOS and hypothyroidism. In both PCOS and Hashimoto’s hypothyroidism, one of the major issues is insulin resistance, which prevents proper sugar metabolism. So, you want to assist your body as much as you can to break the vicious cycle of hormonal imbalances in PCOS and Thyroid.

One way is to manage your sugar levels. A healthy diet for managing both PCOS and thyroid disorders should focus on nutrient-dense, anti-inflammatory foods. Incorporate the following into your meal plan:
- High-fiber fruits and vegetables: Berries, apples, pears, leafy greens, and cruciferous vegetables (cooked to minimize thyroid interference).
- Whole grains: Brown rice, quinoa, whole wheat, oats, and barley.
- Lean proteins: Chicken, turkey, fish (especially those rich in omega-3 fatty acids, like salmon and sardines), and plant-based proteins like beans, lentils, and chickpeas.
- Healthy fats: Avocado, olive oil, nuts, and seeds.
- Dairy alternatives: Opt for unsweetened almond, cashew, or coconut milk instead of soy milk to minimize potential thyroid issues.
- Anti-inflammatory spices and herbs: Turmeric, ginger, cinnamon, and garlic.
- Green tea: Rich in antioxidants, green tea can help reduce inflammation and support weight management.
- Probiotic-rich foods: Yogurt, kefir, sauerkraut, kimchi, and other fermented foods to support gut health and reduce inflammation.
- Hydration: Drink plenty of water and herbal teas to stay hydrated and support overall health.
2. Foods to Avoid with PCOS and Thyroid
To effectively manage PCOS and thyroid disorders, it’s crucial to avoid certain foods that can exacerbate symptoms or negatively affect hormonal balance. Keep the following foods off your plate:
- Refined carbohydrates: White bread, pasta, pastries, and sugary snacks.
- Processed foods: Packaged meals, fast food, and junk food.
- Excessive soy products: Tofu, soy milk, and processed soy-based meat alternatives (consume in moderation).
- Trans fats and hydrogenated oils: Found in margarine, fried foods, and some packaged snacks.
- Added sugars: Sodas, fruit juices, and sugar-laden desserts.
- Alcohol: Excessive alcohol consumption can contribute to hormonal imbalances and inflammation.
- Caffeine: Limit coffee and energy drinks, as they can worsen anxiety and stress, potentially affecting hormonal balance.
- Iodine-rich foods: Excessive iodine intake can exacerbate thyroid issues. Avoid excessive consumption of seaweed, kelp, and iodized salt.
- Raw cruciferous vegetables: In large quantities, raw broccoli, cauliflower, and kale can interfere with thyroid function. Opt for cooked versions instead.
3. Improve your lifestyle to Balance your Hormones
Both PCOS and thyroid disorder significantly affect how your body operates. Hence, you do not want to stress your body further, especially if you have these two conditions to deal with.
- Sleep well. Aim for 7-8 hours of adequate sleep each night
- Regularly practice breathing exercises (pranayama), yoga, and meditation. These activities help you relax from the inside out.
- Exercise is important. Eating healthy alone without exercising will not cut it. However, be careful to not stress yourself out with excessive exercise.
- Manage your stress levels
- Practice self care and take time off on regular intervals
4. Herbal Supplements for PCOS and Thyroid
- Have fenugreek seeds before eating food, that is, on an empty stomach. It is an excellent herb to treat insulin resistance and promote metabolism.
- Licorice root is highly effective for restoring the levels of androgens back to normal. It also helps to regulate cortisol levels and support adrenal gland function, which can be beneficial for both hypothyroidism and PCOS.
- Apply asafoetida (a pinch in warm water)over your stomach during your menstrual cycle. This will help relieve the intense pain that PCOS can cause.
- Coriander and mint juice are highly effective in reducing heat and inflammation inside the body.
- Adaptogens as Shatavari and Ashwagandha are two highly effective Ayurvedic herbs that support your thyroid function and reproductive System.
- Cinnamon is another culinary herb/spice that works well to manage insulin resistance.
- Evening primrose oil contains gamma-linolenic acid (GLA), which helps to reduce inflammation and improve hormone balance in women with PCOS.
- Chaste tree berry, also known as vitex, is helpful to regulate menstrual cycles and improve fertility in women with PCOS.
- Rhodiola is an adaptogenic herb that may help to reduce stress and improve thyroid function, which can be beneficial for managing symptoms of hypothyroidism.
5. Yoga for PCOS and Thyroid
Yoga is a beneficial form of exercise and stress management for women with polycystic ovary syndrome (PCOS) and thyroid disorders. Certain yoga poses, such as forward folds and twists, can help to stimulate the endocrine system and improve hormone balance. In addition, inversions, can help to improve circulation and reduce inflammation, thus helping to treat the two conditions.
Yoga sequence to treat PCOS and Thyroid
The following easy yoga sequence can help manage PCOS and thyroid disorders by promoting relaxation, reducing stress, and improving hormonal balance. Practice these poses regularly for optimal benefits:
- Easy Pose (Sukhasana): Sit comfortably with your legs crossed, spine straight, and hands resting on your knees. Close your eyes and take several deep breaths to center yourself and calm your mind.
- Seated Cat-Cow (Sukhasana with spinal movement): In Easy Pose, place your hands on your knees. Inhale, arch your spine, and lift your chest (Cow). Exhale, round your spine, and tuck your chin towards your chest (Cat). Repeat for 5-10 breaths.
- Seated Forward Bend (Paschimottanasana): Extend your legs in front of you. Inhale, lengthen your spine, and exhale, hinge at your hips, and fold forward over your legs. Hold for 5-10 breaths.
- Butterfly Pose (Baddha Konasana): Sit with the soles of your feet together and knees out to the sides. Inhale, lengthen your spine, and exhale, fold forward over your feet. Hold for 5-10 breaths.
- Bridge Pose (Setu Bandha Sarvangasana): Lie on your back with your knees bent and feet hip-width apart. Inhale, lift your hips and chest towards the ceiling, and clasp your hands underneath your body. Hold for 5-10 breaths.
- Legs-Up-The-Wall Pose (Viparita Karani): Position your mat near a wall. Lie on your back and extend your legs up the wall. Keep your arms relaxed by your sides. Hold for 5-10 minutes, focusing on deep breathing.
- Corpse Pose (Savasana): Lie on your back with your arms resting by your sides, palms facing up. Close your eyes and allow your body to relax completely. Focus on your breath and let go of any tension in your muscles. Stay in this pose for 5-10 minutes, or as long as desired, to conclude your practice.
Conclusion
PCOS and thyroid disorders are two common conditions that can cause a range of symptoms that can impact overall health and well-being. While there is no one-size-fits-all solution for managing these conditions, there are many natural approaches, including diet and lifestyle changes, herbal supplements, and yoga, that can be beneficial for reducing symptoms and improving quality of life.
If you’re struggling with symptoms of PCOS or a thyroid disorder, it’s important to seek help from a qualified healthcare provider who can guide you in developing a personalized treatment plan. In addition to medical treatment, making changes to your diet and lifestyle can be an effective way to manage symptoms and improve overall health.
At Medhya Herbals, we specialize in Ayurvedic medicine, which offers a holistic approach to health and wellness. We can work with you to develop a personalized Ayurvedic treatment plan that incorporates diet, lifestyle modifications, and herbal supplements to support your overall health and well-being. Contact us today to learn more about how Ayurvedic medicine can help you manage symptoms of PCOS and thyroid disorders and improve your quality of life. Take charge of your health today!
FAQ
Can PCOS and Thyroid Patients Get Pregnant?
PCOS and Thyroid patients may find it difficult to get pregnant due to several hormones being in disturbed state. However, it is not impossible!
Since having under functioning thyroid affects your health and your baby’s health during pregnancy, it is important that you discuss your health conditions and your intention to conceive with your gynae. She will be able to advise you on the link between your medications, if you are on any, and how to prepare for a pregnancy.
What is the link between PCOS and hyperthyroidism?
Polycystic ovary syndrome (PCOS) and hyperthyroidism are both endocrine disorders that can impact hormone balance and fertility. However, PCOS is typically associated with hypothyroidism, or an underactive thyroid, rather than hyperthyroidism.
Hyperthyroidism is a condition in which the thyroid gland produces too much thyroid hormone, leading to symptoms such as weight loss, rapid heartbeat, and anxiety. While there is not a direct link between PCOS and hyperthyroidism, some studies have suggested that women with PCOS may be at a higher risk for developing autoimmune thyroid disorders, such as Graves’ disease, which can lead to hyperthyroidism.
Additionally, women with hyperthyroidism may experience irregular menstrual cycles and difficulty conceiving, which can be similar to symptoms of PCOS.
How to Lose Weight with PCOS and Thyroid?
Losing weight with polycystic ovary syndrome (PCOS) and thyroid disorders can be challenging due to hormonal imbalances and other factors that can impact metabolism and appetite. However, it is possible to lose weight with these conditions by making changes to your diet and lifestyle. Here are some tips that may be helpful for losing weight with PCOS and thyroid disorders:
- Focus on nutrient-dense foods: Choose whole, nutrient-dense foods such as vegetables, fruits, whole grains, lean proteins, and healthy fats. Avoid processed and high-sugar foods that can spike blood sugar levels and contribute to inflammation.
- Eat a balanced diet: Aim to balance your meals with a combination of protein, healthy fats, and complex carbohydrates. This can help to regulate blood sugar levels and reduce cravings.
- Limit sugar and refined carbohydrates: Limit your intake of sugar and refined carbohydrates, as these can worsen symptoms of PCOS and thyroid disorders.
- Practice mindful eating: Pay attention to your hunger and fullness cues, and eat slowly and mindfully. This can help you to tune into your body’s needs and prevent overeating.
- Stay active: Regular physical activity can help to boost metabolism and burn calories. Choose activities that you enjoy, such as walking, yoga, or swimming, and aim for at least 30 minutes of activity per day.
- Get enough sleep: Getting enough sleep is important for regulating hormones and managing appetite. Aim for 7-9 hours of sleep per night.
- Work with a healthcare provider: If you are struggling to lose weight with PCOS or thyroid disorders, it’s important to work with a qualified healthcare provider who can guide you in developing a personalized treatment plan.
References
- Zhang Y, Guo X, Guo L, et al. Clinical characteristics and high-risk factors of subclinical hypothyroidism in patients with PCOS: a meta-analysis. Int J Clin Exp Med. 2019;12(7):8831-8838. https://www.ncbi.nlm.nih.gov/pmc/articles/PMC6709838/
- Winder M, Winder C. The polycystic ovary syndrome and thyroid autoimmunity. Clin Endocrinol (Oxf). 2011;74(2):146-151. doi: 10.1111/j.1365-2265.2010.03894.x. https://pubmed.ncbi.nlm.nih.gov/20964740/
- Teede HJ, Misso ML, Costello MF, Dokras A, Laven J, Moran L, Piltonen T, Norman RJ, International PCOS Network. Recommendations from the international evidence-based guideline for the assessment and management of polycystic ovary syndrome. Fertil Steril. 2018;110(3):364-379. doi: 10.1016/j.fertnstert.2018.05.004. https://pubmed.ncbi.nlm.nih.gov/29891267/
- Khomami MB, Tehrani FR, Hashemi S, et al. The prevalence of thyroid dysfunction in polycystic ovary syndrome patients. Biomed Res Int. 2014;2014:508085. doi: 10.1155/2014/508085. https://www.ncbi.nlm.nih.gov/pmc/articles/PMC4028624/
- Diamanti-Kandarakis E, Kandarakis H, Legro RS. The role of genes and environment in the etiology of PCOS. Endocrine. 2006;30(1):19-26. doi: 10.1385/ENDO:30:1:19. https://pubmed.ncbi.nlm.nih.gov/16988415/
- American Thyroid Association. Hypothyroidism (Underactive). https://www.thyroid.org/hypothyroidism/
- American Thyroid Association. Hyperthyroidism (Overactive). https://www.thyroid.org/hyperthyroidism/
- Malik R, Hodgson H. The relationship between the thyroid gland and the liver. QJM. 2002;95(9):559-569. doi: 10.1093/qjmed/95.9.559. https://pubmed.ncbi.nlm.nih.gov/12196612/
- Shalimar, Gupta AK, Bhatia V, et al. Improvement in insulin sensitivity after treatment of non-alcoholic fatty liver disease (NAFLD) with sitagliptin. Diabetes Res Clin Pract. 2016;116:217-224. doi: 10.1016/j.diabres.2016.04.005. https://pubmed.ncbi.nlm.nih.gov/27126379/
- Klibanski A. Clinical practice. Amenorrhea. N Engl J Med. 2010;363(14):1379-1386. doi: 10.1056/NEJMcp1001110. https://pubmed.ncbi.nlm.nih.gov/20925550/
- Thyroid Disorders in Women with Polycystic Ovary Syndrome

