Are you aware that not all cases of PCOS are the same? Polycystic Ovary Syndrome, commonly known as PCOS, is a complex and often misunderstood condition. It comes in various forms, each with its unique characteristics and symptoms. In our quest for better health, it’s crucial to recognize that being informed is the first step toward understanding your body and taking control of your well-being.
In this blog post, we delve into the world of PCOS, exploring the four distinct types of PCOS and the telltale signs and PCOS symptoms that should not be ignored. Understanding these nuances can be the key to proactive management, ensuring that you receive the right care and support for your specific PCOS subtype. So, let’s unravel the mysteries of these PCOS variations and empower ourselves with knowledge about types of PCOS and the symptoms that warrant attention.
What is PCOS?
PCOS is a common condition that affects many women of reproductive age. It’s caused by hormonal imbalances in the body, leading to problems with ovulation and increased levels of male hormones.
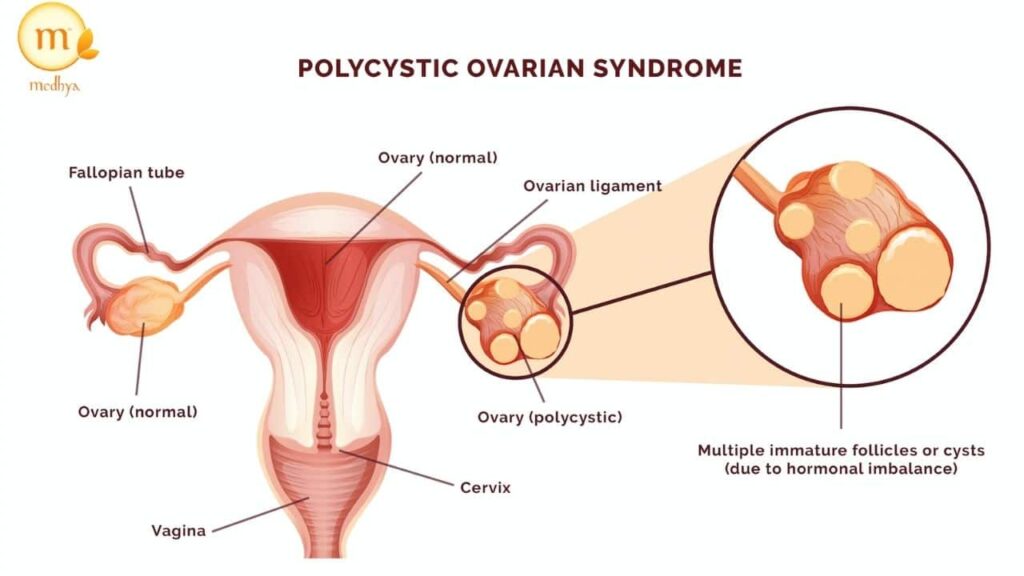
The name “polycystic” is a bit misleading, as it refers to multiple underdeveloped follicles (not cysts) on the ovaries that are commonly seen on a pelvic ultrasound. These follicles are supposed to release an egg for fertilization, but in PCOS, they often get stuck in their development.
As a result, many women with PCOS struggle to ovulate on time. It’s worth noting that not all women with PCOS have polycystic ovaries, and diagnosis doesn’t necessarily require their presence.

The Types of PCOS: Which One do You Have?
There are four types of PCOS: Adrenal PCOS, Insulin-resistant PCOS, Inflammatory PCOS and Pill-induced PCOS that I encounter at my clinic. Understanding the different types of PCOS is essential in determining the best treatment approach. Let’s look into causes and symptome of each type of PCOS:
Adrenal PCOS
Adrenal PCOS is caused by high levels of androgens, male hormones produced by the adrenal gland. This type of PCOS is characterised by symptoms such as excess hair growth, acne, and irregular periods. Ayurvedic treatment for Adrenal PCOS often involves balancing the levels of androgens in the body through herbal remedies and lifestyle changes.
Insulin-resistant PCOS
Insulin resistant PCOS is the most common type of PCOS. It occurs when the body is resistant to insulin, leading to high levels of insulin in the bloodstream. This excess insulin can cause the ovaries to produce more androgen, leading to symptoms such as weight gain, hair loss, and acne. Ayurvedic treatment for PCOS and Insulin Resistance often involves dietary changes and herbal remedies that can help balance blood sugar levels and reduce inflammation in the body.
Inflammatory PCOS
Inflammatory PCOS is characterised by inflammation in the body that can lead to insulin resistance and androgen excess. This type of PCOS is often accompanied by symptoms such as acne, hair loss, and weight gain. Ayurvedic treatment for Inflammatory PCOS often involves anti-inflammatory herbs and dietary changes that can help reduce inflammation in the body and balance hormone levels.
Pill-induced PCOS
Pill-induced PCOS occurs when a woman stops taking birth control pills. The pills contain hormones that regulate the menstrual cycle and prevent the ovaries from producing cysts. When a woman stops taking the pill, her body may take time to adjust, leading to the formation of cysts on the ovaries. Ayurvedic treatment for Pill-induced PCOS often involves herbal remedies and dietary changes that can help regulate the menstrual cycle and support the body’s natural hormonal balance.
PCOS Symptoms Checklist
PCOS presents itself in different ways in different women. You may experience one or more of the health symptoms listed below. Also, the extent to which a health symptom is present in a women varies depending on her hormone imbalances.
For example, if you are experiencing high levels of Androgens or male hormones, then you will constantly struggle with Irregular periods, facial hair, acne, and hair loss on scalp.
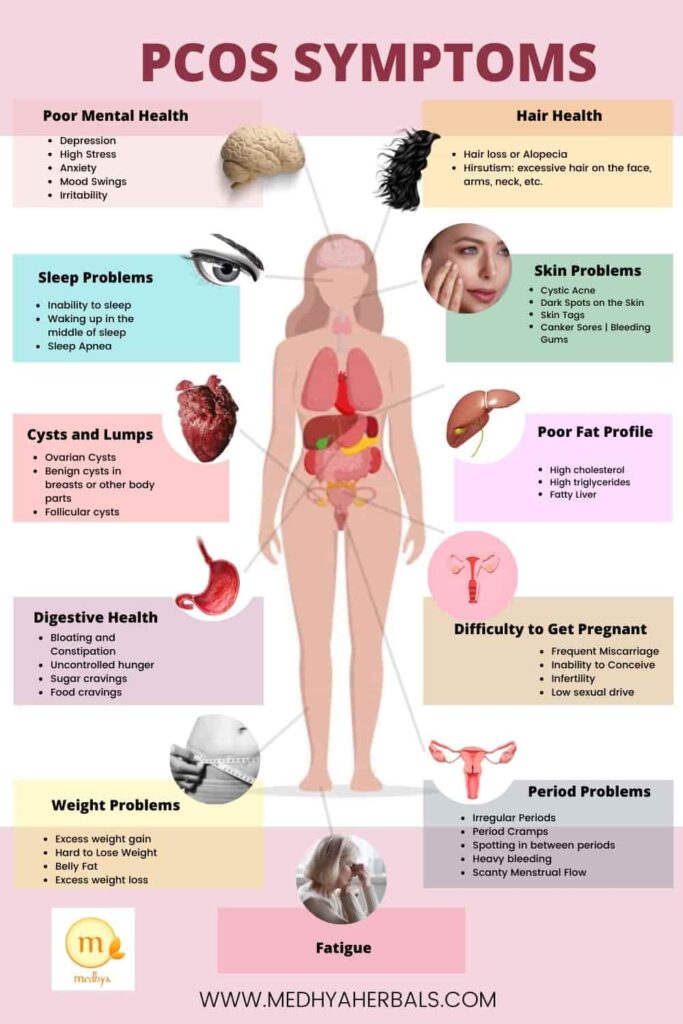
Here ‘s PCOS Symptoms Checklist for you to know whether you fall in the risk category of having PCOS.
- PCOS Fertility Issues
- Frequent Miscarriage
- Inability to Conceive
- Infertility
- Low sexual drive
- Cysts on the Ovaries
- Period Problems
- Irregular Periods
- Period Cramps
- Spotting in between periods
- Heavy bleeding
- Scanty Menstrual Flow
- Weight Problems
- Excess weight gain
- Belly Fat
- Excess weight loss
- Metabolic syndrome
- Skin Problems
- Acne
- Dark Spots on the Skin
- Dark neck, underarms and dark skin in inner thighs
- Skin Tags
- Hair Health
- Poor Mental Health
- Depression and anxiety
- High Stress
- Mood Swings
- Irritability
- Fatigue
- Digestive Issues
- Bloating and Gas
- Constipation, Indigestion and sluggish bowel movement
- Uncontrolled hunger
- Food cravings in specific sugar cravings
- Poor Fat Profile
- Sleep Problems
- Inability to sleep
- Waking up in the middle of sleep
- Sleep Apnea
- Hormone Imbalances
- High Androgens
- High LH
- Low FSH
- Low Progesterone
- Estrogen Dominance
- Insulin resistance and High Insulin levels
- High Cortisol
What are the First Signs of PCOS?
PCOS, or Polycystic Ovary Syndrome, can manifest in different ways, and the symptoms can vary from woman to woman. Some women may experience only a few of the symptoms, while others may have several. Here are some of the first signs of PCOS that you should look out for:
- Irregular periods: One of the most common signs of PCOS is irregular periods. This can mean having fewer periods than normal, having periods that last longer than usual, or having periods that are very light or very heavy.
- Acne: Women with PCOS may experience acne, especially on their face, chest, and back. This is due to the increased production of androgens, male hormones that can cause excess oil production and inflammation in the skin.
- Excess hair growth: PCOS can cause excess hair growth on the face, chest, back, and stomach. This condition is called hirsutism and is caused by the increased production of androgens.
- Weight gain: Women with PCOS may find it difficult to lose weight, and may gain weight easily. This is due to the insulin resistance that is often associated with PCOS.
- Hair loss: PCOS can cause hair loss on the scalp, which is due to the increased production of androgens.
What are the Causes of PCOS?
The exact causes of PCOS, or Polycystic Ovary Syndrome, are not fully understood, but it is believed to be a combination of genetic, hormonal, and lifestyle factors.
- Genetics: PCOS can run in families, and certain genes may increase a woman’s risk of developing the condition. However, the specific genes involved in PCOS have not yet been identified.
- Hormonal Imbalance: PCOS is a hormonal disorder, and it is believed that imbalances in certain hormones can contribute to the development of the condition. Women with PCOS typically have higher than normal levels of androgens, male hormones that are also present in women. This excess of androgens can cause the ovaries to produce more follicles than normal, which can lead to the formation of cysts.
- Insulin Resistance: Insulin is a hormone that helps regulate blood sugar levels in the body. Women with PCOS are often insulin resistant, which means that their bodies are less able to use insulin effectively. This can lead to high levels of insulin in the bloodstream, which can cause the ovaries to produce more androgens, leading to symptoms such as acne, excess hair growth, and weight gain.
- Inflammation: Inflammation is a natural response of the body to injury or infection. However, chronic inflammation can contribute to the development of PCOS. Women with PCOS often have higher levels of inflammation in their bodies, which can contribute to insulin resistance and androgen excess.
- Lifestyle factors: Lifestyle factors such as diet and exercise can also contribute to the development of PCOS. A diet high in refined carbohydrates and sugars can lead to insulin resistance, while lack of exercise can contribute to weight gain and inflammation.
PCOS Diagnosis | How do you Know When you have PCOS?
Diagnosing PCOS, or Polycystic Ovary Syndrome, can be challenging as there is no single test that can confirm the condition. Instead, healthcare providers use a combination of tests and evaluations to determine if a woman has PCOS.
The diagnostic criteria for PCOS vary slightly depending on the medical organization, but most healthcare providers follow the Rotterdam criteria. According to these criteria, a woman must have at least two of the following three criteria to be diagnosed with PCOS:
- Irregular periods: Women with PCOS may have fewer than eight periods per year or have periods that are very long, very short, or very light.
- Androgen excess: Women with PCOS may have high levels of androgens, male hormones that are also present in women. Androgen excess can lead to symptoms such as acne, excess hair growth, and hair loss.
- Polycystic ovaries: Women with PCOS may have multiple cysts on their ovaries, which can be seen on an ultrasound.
Diagnosing PCOS requires a combination of tests and evaluations:
- Medical history: Healthcare providers will ask about your menstrual cycle, symptoms, and family history of PCOS or other hormonal disorders.
- Physical exam: Healthcare providers may perform a physical exam to check for signs of androgen excess, such as excess hair growth, acne, and hair loss.
- Blood tests: Blood tests can be used to check hormone levels, including androgens, estrogen, and progesterone. Blood tests can also be used to check for other conditions that can cause similar symptoms, such as thyroid disorders.
- Ultrasound: An ultrasound can be used to check for the presence of cysts on the ovaries. However, it’s important to note that not all women with PCOS have cysts on their ovaries, and not all women with cysts on their ovaries have PCOS.
If you suspect you have PCOS, it’s important to speak with your healthcare provider to discuss your symptoms and determine the best course of action for diagnosis and treatment.
Health Risks of Untreated PCOS
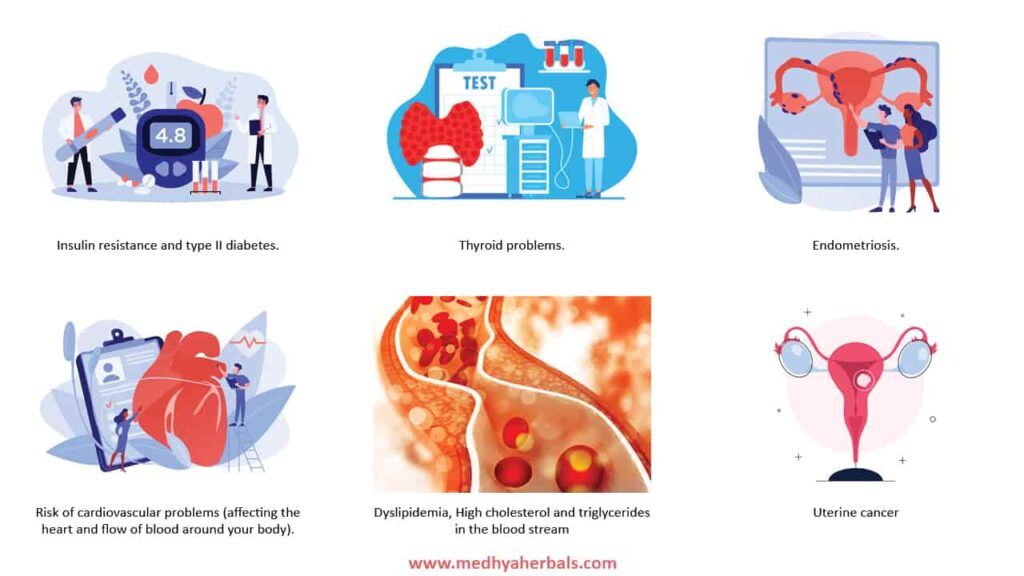
PCOS is a progressive health disorder. If left untreated, PCOS (Polycystic Ovary Syndrome) can lead to several health complications. Some of these complications are:
- Infertility: PCOS can make it difficult for women to conceive, as it can cause irregular periods and anovulation (lack of ovulation). This can make it harder to predict ovulation and time intercourse for optimal chances of pregnancy.
- Diabetes: Women with PCOS are at higher risk of developing type 2 diabetes due to insulin resistance. Insulin resistance can cause elevated blood sugar levels and can eventually lead to diabetes if left untreated.
- Cardiovascular disease: Women with PCOS are at higher risk of developing cardiovascular disease, including high blood pressure, high cholesterol, and heart attacks. This is due to the increased insulin resistance and inflammation associated with PCOS.
- Endometrial cancer: Women with PCOS are at higher risk of developing endometrial cancer, a type of cancer that affects the lining of the uterus. This is due to the excess of estrogen that can occur in women with PCOS who do not ovulate regularly.
- Sleep apnea: PCOS is also associated with sleep apnea, a condition where breathing stops and starts during sleep. Sleep apnea can lead to daytime fatigue and other health complications.
- Depression and anxiety: PCOS can have a significant impact on a woman’s mental health. Women with PCOS are at higher risk of developing depression and anxiety due to the impact of the condition on their physical health, fertility, and overall quality of life.
Conclusion
Breaking the cycle is key to find relief from PCOS Symptoms!
Now, you have seen PCOS symptoms and gotten a pretty good understanding of the causes and triggers behind your health issues. If you’ve been following well, you would have noticed that there are patterns and cycles that are based on the causes of PCOS.
A good number of the problems link up to high Androgens or high insulin levels in your body. From here, there are chain reactions that cause the symptoms. In many cases, one of the symptoms cause other symptoms or come back and worsen off the root causes of hormone imbalance.
Are you ready to break the cycle? I bet you are. You can start by checking how to regulate what you eat by adopting PCOS Diet and by checking our post on PCOS Ayurvedic Treatment.
Your journey to beat PCOS starts now!
FAQ
What Causes PCOS Cysts to Grow?
The term “polycystic” refers to multiple cysts, but it was used to describe the appearance of multiple follicles on the ovaries in women with PCOS as seen on a pelvic ultrasound. However, these follicles are not actually cysts, but rather underdeveloped follicles that do not release an egg during ovulation.
PCOS Cysts are caused by problems with ovulation, which results in these follicles getting stuck in their development. Normally, up to 12 follicles begin to develop at once, with one becoming the dominant follicle that releases an egg for fertilization during ovulation.
But in women with PCOS, the follicles may not progress to the final stage of development, leading to difficulty in ovulation. As a result, women with PCOS may struggle to ovulate on time, causing hormonal imbalances and other symptoms associated with the condition.
What are the signs of insulin resistance PCOS?
Insulin resistance is a common feature of polycystic ovary syndrome (PCOS) and can contribute to the development of other symptoms associated with the condition. Some signs of insulin resistance in PCOS may include:
- Weight gain or difficulty losing weight
- High blood sugar levels or pre-diabetes
- Fatigue and low energy levels
- Skin changes such as darkening or thickening, especially around the neck or armpits
- Increased hunger or cravings for sugary foods
- Irregular menstrual cycles or absence of periods
- Excess hair growth on the face, chest, or stomach
- Acne or other skin problems
- Mood swings or depression.
PCOS vs PCOD | What’s the Difference?
PCOS and PCOD are two terms that are often used interchangeably, leading to confusion. However, while they share some similarities, they are slightly different conditions.
PCOS, or Polycystic Ovarian Syndrome, is a hormonal disorder that affects the ovaries. It occurs when the body produces too much androgen, leading to symptoms such as acne, excess hair growth, and irregular periods. Women with PCOS may also develop cysts on their ovaries, hence the name Polycystic Ovarian Syndrome. PCOS can lead to fertility issues and other health problems, such as insulin resistance and diabetes.
PCOD, or Polycystic Ovary Disease, is a condition where multiple cysts develop on the ovaries, leading to irregular periods and fertility issues. PCOD is often confused with PCOS, but they are not the same. While PCOS can cause cysts to form on the ovaries, not all women with PCOS develop cysts. Similarly, not all women with PCOD have the hormonal imbalances associated with PCOS.
One of the main differences between PCOS and PCOD is the way they are diagnosed. PCOS is diagnosed based on a combination of symptoms, such as irregular periods and excess hair growth, and the presence of cysts on the ovaries. PCOD, on the other hand, is diagnosed based on the presence of cysts on the ovaries and irregular periods.
Are PCOS and endometriosis the same?
No, PCOS and endometriosis are not the same condition. While they can both affect a woman’s reproductive health and cause similar symptoms, they are two distinct conditions with different causes and treatments.
PCOS, or Polycystic Ovary Syndrome, is a hormonal disorder that affects the ovaries. It is characterized by the presence of cysts on the ovaries, irregular periods, and excess levels of androgens, male hormones that are also present in women. PCOS can cause symptoms such as acne, hair loss, weight gain, and fertility issues.
Endometriosis, on the other hand, is a condition where tissue similar to the lining of the uterus grows outside of the uterus, causing pain and discomfort. The tissue can grow on the ovaries, fallopian tubes, and other organs in the pelvis. Endometriosis can cause symptoms such as painful periods, pain during sex, and fertility issues.
Check out here Ayurvedic treatment for Endometriosis.
What are the hormone levels for PCOS?
Hormone levels can vary widely among women with the condition. However, certain hormonal imbalances are commonly observed in PCOS, such as:
- Elevated androgen levels: Testosterone levels greater than 2.7 nmol/L (78 ng/dL) and/or DHEAS levels greater than 4,500 ng/mL are often considered high and may suggest PCOS.
- Elevated LH levels: Women with PCOS may have LH levels that are higher than FSH levels, or a ratio of LH to FSH greater than 2:1.
- Insulin resistance: Fasting insulin levels greater than 15-20 microU/mL or a homeostatic model assessment for insulin resistance (HOMA-IR) greater than 2.5 are often used as markers for insulin resistance, which is common in women with PCOS.
It’s important to note that hormone levels alone are not sufficient to diagnose PCOS, and a combination of symptoms, physical exam, and laboratory testing is typically used to make a diagnosis.
What comes first PCOS or insulin resistance?
The relationship between polycystic ovary syndrome (PCOS) and insulin resistance is complex and not fully understood. It is not clear which condition comes first, as they may develop concurrently or influence each other.
Some researchers suggest that insulin resistance may be an underlying factor in the development of PCOS, as it can contribute to the overproduction of androgens (male hormones) by the ovaries, leading to hormonal imbalances and other symptoms of PCOS.
On the other hand, others suggest that PCOS may lead to insulin resistance, as the hormonal imbalances associated with PCOS can affect the body’s ability to use insulin effectively, leading to higher insulin levels and insulin resistance.
It’s important to note that the relationship between PCOS and insulin resistance may vary among women and may depend on individual factors such as genetics, lifestyle, and environmental factors.
What does inflammation in PCOS mean?
Inflammation refers to the body’s response to injury, infection, or tissue damage. In the case of polycystic ovary syndrome (PCOS), inflammation may play a role in the development and progression of the condition.
Research suggests that women with PCOS may have higher levels of inflammation in the body, as evidenced by higher levels of certain markers such as C-reactive protein (CRP) and interleukin-6 (IL-6).
This inflammation may contribute to insulin resistance, as well as other metabolic and cardiovascular risks associated with PCOS. It may also affect ovarian function and contribute to the development of cysts or follicular abnormalities seen in PCOS.
How do I know my PCOS is getting better?
Polycystic ovary syndrome (PCOS) is a complex condition that can manifest in different ways for different individuals. Generally, there are a few signs that your PCOS may be improving:
- Regular menstrual cycle: One of the hallmarks of PCOS is irregular menstrual cycles or periods. If you start to experience more predictable cycles, this could be a sign that your PCOS is improving.
- Improved fertility: PCOS can affect fertility in some individuals. If you are trying to conceive, an improvement in fertility could be a sign that your PCOS is getting better.
- Decrease in symptoms: Symptoms of PCOS can vary, but common ones include acne, excess hair growth, and weight gain. If you notice a decrease in these symptoms, it could indicate that your PCOS is improving.
- Blood test results: PCOS can cause hormonal imbalances, including high levels of androgens and insulin resistance. If your blood test results show improvement in these areas, it could be a sign that your PCOS is getting better.
Can adrenal issues cause PCOS?
Adrenal issues, such as adrenal hyperplasia or adrenal tumors, can sometimes cause symptoms that are similar to polycystic ovary syndrome (PCOS), such as hirsutism (excess hair growth) and irregular periods. However, adrenal issues alone are not typically considered a cause of PCOS.
What foods help adrenal PCOS?
There is no specific diet that has been shown to cure or treat adrenal PCOS. However, some dietary changes may be helpful in managing symptoms and improving overall health in women with PCOS, including those with adrenal issues. Here are some tips for a healthy PCOS diet:
- Choose complex carbohydrates: Complex carbohydrates such as whole grains, fruits, and vegetables can help regulate blood sugar levels and reduce insulin resistance, a common feature of PCOS.
- Increase protein intake: Eating protein at each meal can help keep you feeling full and satisfied and may help regulate blood sugar levels.
- Include healthy fats: Healthy fats such as omega-3 fatty acids found in fatty fish, nuts, and seeds can help reduce inflammation in the body.
- Avoid processed foods and added sugars: Processed foods and added sugars can contribute to insulin resistance and inflammation, which can exacerbate PCOS symptoms.
- Consider supplements: Certain supplements such as vitamin D, inositol, and magnesium may be beneficial for women with PCOS, but it’s important to speak with your healthcare provider before taking any supplements.
References
- Polycystic ovary syndrome
- AN EFFORT TO UNDERSTAND PCOS IN AYURVEDA CONTEXT
- Concept of Polycystic Ovarian Syndrome: Perspectivesof Ayurvedaand ModernScience
- Centers for Disease Control and Prevention. PCOS (polycystic ovary syndrome) and diabetes.
- Goyal M, Dawood AS. Debates regarding lean patients with polycystic ovary syndrome: A narrative review. J Hum Reprod Sci. 2017;10(3):154‐161. doi:10.4103/jhrs.JHRS_77_17
- Pelanis R, Mellembakken JR, Sundström-Poromaa I, et al. The prevalence of Type 2 diabetes is not increased in normal-weight women with PCOS. Hum Reprod. 2017;32(11):2279-2286. doi:10.1093/humrep/dex294

